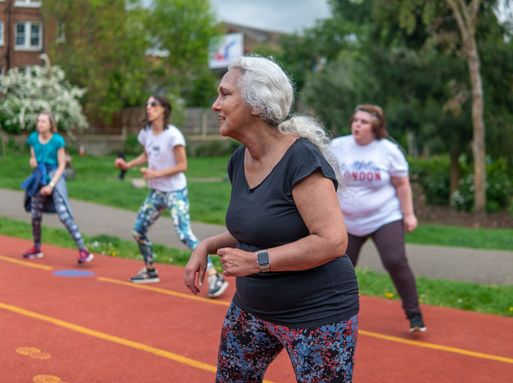As the third-largest workforce in the NHS, Allied Health Professions work across a range of valuable areas of health and wellbeing. This hub is designed to provide information, encourage best practice and tell success stories of professionals who do incredible work every day to protect and improve the public's health.
The hub was created through a collaboration between RSPH, the Office for Health Improvement and Disparities, the Welsh Government, the Northern Ireland Government, the Scottish Government, the Public Health Agency, and key partner organisations.
What are the Allied Health Professions?
There are 14 Allied Health Professions in total: Art therapists, Dietitians, Dramatherapists, Music therapists, Occupational therapists, Operating department practitioners, Orthoptists, Osteopaths, Paramedics, Physiotherapists, Podiatrists, Prosthetists and orthotists, Radiographers and Speech and language therapists.
Allied Public Health Role Descriptors
These descriptions, and the accompanying handbook, highlight AHP contributions across the four key domains of public health. They focus on where and how AHP support worker roles can influence and improve the public’s health and encourage the reader to reflect on their current and potential roles and responsibilities.
Read more
Allied Health Professional case studies
Our Allied Health Professional case studies show how innovative programmes, service design, quality improvement and training can have a positive effect on the public's health and wellbeing. We are always open to hearing about and publishing public health initiative case studies.
Discover valuable resources and reports
These resources, reports and papers have been created to help Allied Health Professionals to further the impact of their contributions to the health of the four nations.
Read more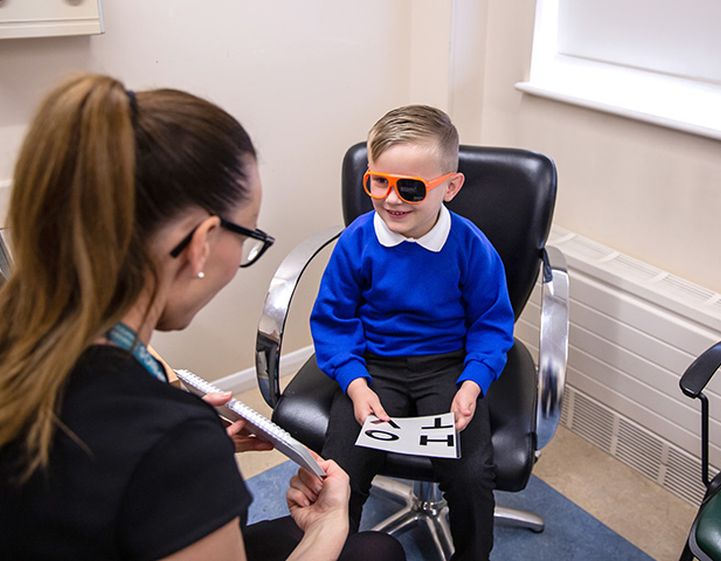
Find out more about Allied Health Professions
For more information about Allied Health Professions, visit the NHS england website.
Make connections with RSPH membership
RSPH membership helps you to network with other members, learn through free online courses and journal access, and show your credentials through post-nominals.
Become a member